Business rules and edits
The SCE has a series of modules that are used in the orchestration to improve the accuracy of the claim and to set the claim up to run cleanly through the benefit adjudication capabilities.
These features include applying specific business and clinical edits and audits to the claim, splitting the claim when necessary and checking the claim against the coordination of benefits (COB) rules. The goal of this step is to ensure that the claim has all the correct data and is organized to adjudicate against benefits and pricing information cleanly.
Smart Claims Engine provides multiple modules to apply business logic to determine if the claim should be suspended for review or denied before it starts adjudication. This logic is applied in two different modules: Business Edits (validating information on the current claim against rules) and Business Audits (validating information against other claims and historical data to apply business rules).
The types of edits are listed below:
- Dynamic Events - Smart Claims Engine provides a utility to create event
logic through the user interface, enabling a business analyst to configure a
business edit using key fields and data on the claims.

- Timely Filing - Smart Claims Engine provides the ability to apply timely filing rules based on a state, contract, federal rule, and system default.
- PCP Required – Smart Claims Engine provides the ability to configure plans and networks that require a PCP to validate the providers on the claim.
- Exact and Suspect Duplicate Claim – Smart Claims Engine provides the capability to identify suspect and exact duplicate claims, and to trigger event codes based on the results. Duplicate logic can be applied within the current claim or against historical claims. The fields used for matching for the duplicate checks are configurable by the Business Analyst.
- Fraud and Abuse – Smart Claims Engine provides a base fraud and abuse table for an end user to configure attributes that would raise an event code on the claim to allow for pre-payment review.
- Interim Bill – Smart Claims Engine provides logic to ensure all pieces of an interim bill are identified before the final claim is paid. This application allows the user to manage institutional interim bills, so that multiple claims for a period of service dates can be adjudicated in the proper sequence.
- Hospital Readmission - Smart Claims Engine identifies unplanned hospital readmissions based on user defined criteria. Decision tables and data transforms help define and apply criteria to include or exclude readmission candidates. The claims engine identifies suspect claims in the patient’s history, and readmissions may be resolved by waiving copayments and repricing claim lines.
- National Correct Coding Initiative (NCCI) Edits - Smart Claims Engine can execute the NCCI Medically Unlikely Edit (MUE), which compares the units of service on the claim with the maximum units of service in the definition table. The application can also execute the NCCI Procedure to Procedure Edit (PTP), which ensures that certain procedures cannot be billed together by the same provider on the same day. Claim modifiers can be configured and used to override the PTP event code. The files containing the code combinations, override rules, and maximum units to support the NCCI edits are provided by the Centers for Medicare & Medicaid Services (CMS).
- Dental Pre-Determination – Smart Claims Engine can look to see if a pre-determination dental claim has been submitted previously and can be matched to the current claim.
Smart Claims Engine is packaged with coordination of benefits (COB) or Third-party liability (TPL) edits to identify if another payer should be responsible for this claim prior to it being adjudicated. The SCE supports both medical other insurance and non-medical insurance subrogation. Information on the claim, coupled with known member policy information, is used to identify the order of payers and then the previous payer adjustments submitted on the claim are used to validate that the other payer(s) have contributed appropriately to the payment. In the instance the other payers have not contributed to the claim, the SCE will set event codes to deny or suspend based on their configuration. The order of other insurance policies to be applied on the claim are configurable. The types of diagnosis codes and claim indicators to configure a non-medical subrogation review are configurable. The SCE provides a guided flow for resolving subrogation claims.
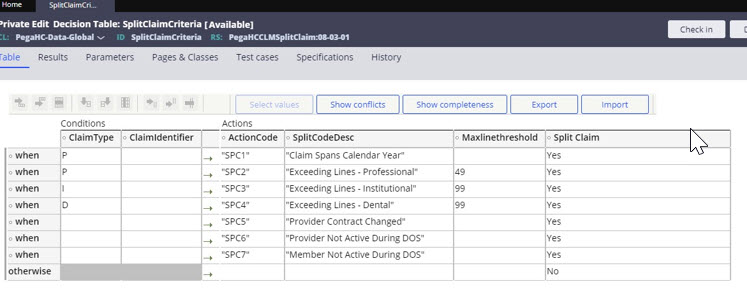
Split claimsThe SCE provides rules to automatically split a claim when necessary for processing. The SCE can also split a claim line. The following scenarios have been implemented to support the splitting of claims.
- Calendar year-based split – Where a claim spans multiple calendar years.
- Provider contract – Where the claim spans multiple provider contracts, or the provider is not active during the claim dates of service.
- Member policy – Where the claim spans multiple sequential policies or the member’s eligibility is terminated during the claim dates of service.
- Number of claim lines – Where the claim exceeds a set number of lines. This can be differentiated between claim types.
The claims split logic is configurable and extensible as required based on customer business rules. There are also configurable rules on when a claim may not be eligible for splitting based on the scenarios detailed above.
Smart Claims Engine provides an out of the box adaptor to integrate with ClaimsXten software. With this seamless integration, clients can auto-adjudicate medical policy claim edits and simplify the management of complex clinical and reimbursement rules. The integration supports real-time claims editing, automatic response handling, appending, and denying claim lines, and applying allowable price reductions.
Previous topic Pre-adjudication Next topic Coverage determination
