Appeal - UC 6: Clinical review of appeal information
Pega Foundation for Healthcare
- Retrieve the case from NurseReview@MyHealthPlan workbasket.

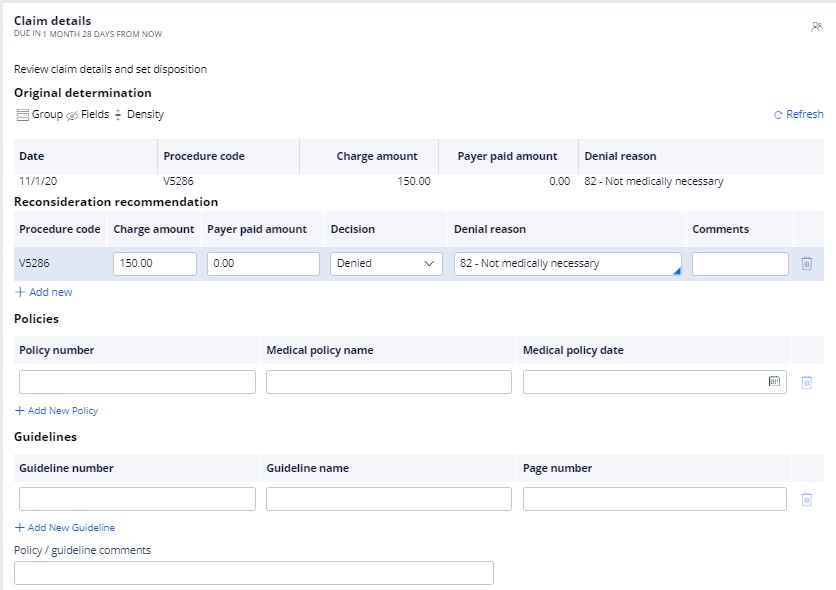
- System displays following Claim line information for each line in the claim:
- Service Date
- Procedure Code
- Charge Amount
- Payer paid amount
- Denial reason
- Edit Patient paid amount and denial reason to deny reconsideration.
- Enter Guideline/Policy reference used for reconsideration. The following
Guideline/Policy reference information can be entered:
- Policy Number
- Medical Policy Date
- Medical Policy name
- Guideline number
- Guideline name
- Page number
User can enter multiple guidelines and policy details. User may decide to route an appeal to any of the following workbaskets:
- RequestAdditionalInformation
- TransferToManager
- TransferToUM (Utilization Manager)
- TransferToCR (claims Review)
In this case, the reviewer routes the case to any of the above workbaskets, and the system provides facility to add the forwarding comment before the case can be forwarded to the workbasket.
- Select disposition.
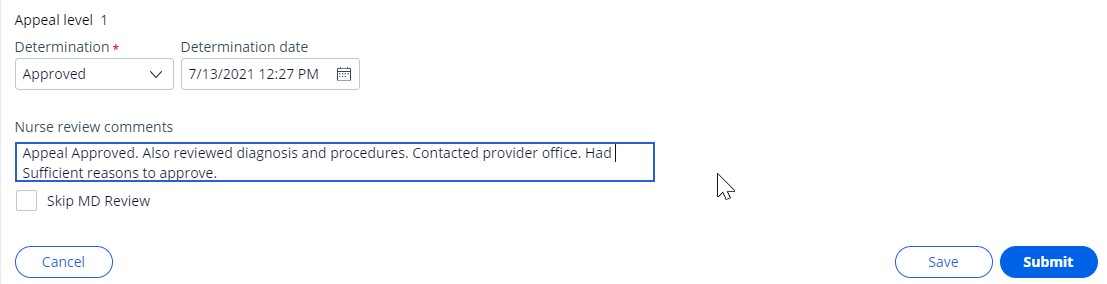
- Edit comments and click ‘Submit’ to record Nurse Review’s disposition.
- Nurse review data is saved and is made available during MD review.
- The system moves the case to MDReview@MyHealthPlan workbasket for MD review.
Previous topic Appeal - UC 5: Review and research appeal information Next topic Appeal - UC 7: Perform medical review of an appeal
